Complex Regional Pain Syndrome
What is complex regional pain syndrome?
Complex regional pain syndrome (CRPS) is a chronic pain condition typically affecting an upper or lower limb. There are two main types: CRPS type 1 (formerly known as reflex sympathetic dystrophy or RSD) occurs after injury or illness but without focal nerve injury while CRPS type 2 (formerly known as causalgia) occurs in the setting of a distinct nerve injury. See below for typical symptoms and signs of CRPS.
What causes complex regional pain syndrome?
Etiologies of CRPS may include trauma, orthopedic injuries (bone fractures, ligament sprains, etc.), postoperative complications, peripheral nerve injuries, cardiovascular events (heart attack, stroke), and inflammatory processes. However, 10-20% of cases of CRPS may occur without a known precipitating cause.
How is complex regional pain syndrome diagnosed?
In order to make a precise diagnosis of CRPS, the following criteria must be met (Harden et al. Complex Regional Pain Syndrome: Practical Diagnostic and Treatment Guidelines, 4th Edition. Pain Medicine 2013; 14: 180-229):
- Continuing pain, which is disproportionate to any inciting event
- Patient must report at least one symptom in three of the four following categories:
- Sensory: Reports of hyperalgesia (increased pain from a stimulus that normally provokes pain) or allodynia (pain due to stimulus that does not normally provoke pain)
- Vasomotor: Reports of temperature asymmetry and/or skin color changes and/or skin color asymmetry
- Sudomotor/Edema: Reports of edema and/or sweating changes and/or sweating asymmetry
- Motor/Trophic: Reports of decreased range of motion and/or motor dysfunction (weakness, tremor, dystonia) and/or trophic changes (hair, nail, skin)
- Patient must display at least one sign (observed at time of diagnosis) in two or more of the following categories:
- Sensory: Evidence of hyperalgesia (to pin prick) and/or allodynia (to light touch and/or deep somatic pressure and/or joint movement)
- Vasomotor: Evidence of temperature asymmetry and/or skin color changes and/or asymmetry
- Sudomotor/Edema: Evidence of edema and/or sweating changes and/or sweating asymmetry
- Motor/Trophic: Evidence of decreased range of motion and/or motor dysfunction (weakness, tremor, dystonia) and/or trophic changes (hair, nail, skin)
- There is no other diagnosis that better explains the signs and symptoms
How is complex regional pain syndrome treated?
Initial treatment options may include analgesic medications, physical therapy, occupational therapy, chiropractic, or functional restoration program. Interventional options include stellate ganglion block for upper limb CRPS or lumbar sympathetic block for lower limb CRPS. Finally, if the patient has tried typical conservative measures but has not noted significant improvement in pain and function, a spinal cord stimulator trial can then be considered.
Stellate Ganglion Block
A stellate ganglion block involves injecting local anesthetic at the sympathetic nerves located at the anterior (front) aspect of the neck. The aim of a stellate ganglion block is to reduce the pain of upper limb CRPS. Using fluoroscopic (x-ray) or ultrasound guidance, a needle is safely and precisely guided to the location of the stellate ganglion. Local anesthetic is then administered to block these nerves and reduce arm pain. Common side effects of the procedure include a warm feeling of the upper limb, hoarse voice, “lump in throat” sensation, droopy eye (ptosis), decrease in sweating of face (anhidrosis), and constriction of the pupil (miosis).
Lumbar Sympathetic Block
A lumbar sympathetic block involves injecting local anesthetic at the sympathetic nerves located at the anterolateral aspect (just in front and off to the side) of the lumbar vertebral bodies. The aim of a lumbar sympathetic block is to reduce the pain of lower limb CRPS. Using fluoroscopic (x-ray) guidance, a needle is safely and precisely guided to the location of the lumbar sympathetic nerves. Local anesthetic is then administered to block these nerves and reduce leg pain. Common side effects of the procedure include a warm feeling of the lower limb as well as possible temporary weakness or numbness of the lower limb.
Spinal Cord Stimulator
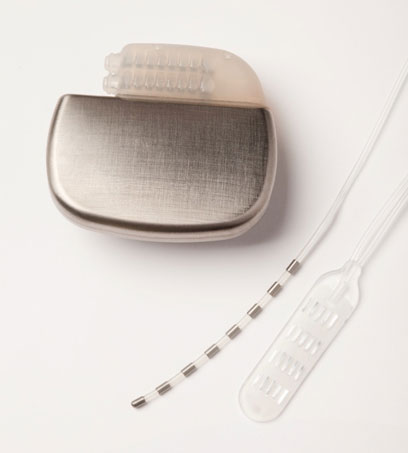
A spinal cord stimulator (SCS) is a non-surgical, minimally invasive treatment for CRPS that uses electrical impulses to block specific nerves of the spinal cord that transmit pain. It consists of a pacemaker-like battery pack called a generator and thin wires called leads. Together, the generator and leads produce electrical signals that stimulate specific nerves of the spinal cord which mask or modify pain signals before reaching the brain, thus greatly diminishing a person’s interpretation and perception of pain.
SCS may be used for patients who have chronic pain conditions despite trials of treatment options such as medications, physical therapy, chiropractic, injections, and even surgery. Indications for use of SCS include chronic low back or neck pain with or without limb pain such as failed back surgery syndrome (post-laminectomy pain syndrome). It may also be used for patients with chronic nerve pain conditions such as complex regional pain syndrome (CRPS), painful peripheral polyneuropathy, or painful diabetic neuropathy. Finally, SCS may be used for those patients with chronic pain who may not be surgical candidates or those who wish to avoid surgery altogether.
If a patient is deemed to be a good candidate for a SCS, Dr. Best will discuss performing a trial first. During a SCS trial, the epidural space is accessed using an introducer needle and x-ray (fluoroscopic) guidance just like an epidural steroid injection. However, rather than instilling steroid through the needle, a very small and thin wire (spinal cord stimulator lead) is inserted into the epidural space and gradually advanced to the mid-thoracic region. The other end of the leads exit the skin at the site oof introducer needle placement and connected to the generator which will be secured to the patient’s flank area during the 5–7-day trial period. During this 5–7-day period, the patient has the opportunity to test out the SCS technology and get a sense of whether it helps to significantly decrease pain and improve function. The patient then returns to Dr. Best’s clinic to discuss the result of the SCS trial. During the follow up visit in clinic, the SCS trial leads are removed and, if successful, the patient may choose to have the spinal cord stimulator permanently placed. When a SCS is placed on a permanent basis, all components of the leads are once again placed in the epidural space and advanced to the mid-thoracic region; however, they are then tunneled under the skin and connected to the generator which is sitting in a subcutaneous pocket created with a small incision.
The common goals when considering the use of SCS include significantly decreasing pain, decreasing need for and use of pain medication, and improvement in overall function.
At a Glance
Dr. Craig Best
- Harvard Fellowship-Trained Interventional Spine & Sports Medicine Specialist
- Double Board-Certified in Physical Medicine & Rehabilitation and Pain Medicine
- Assistant Professor of Physical Medicine & Rehabilitation and Orthopedic Surgery
- Learn more

