Knee Arthritis
What is knee arthritis?
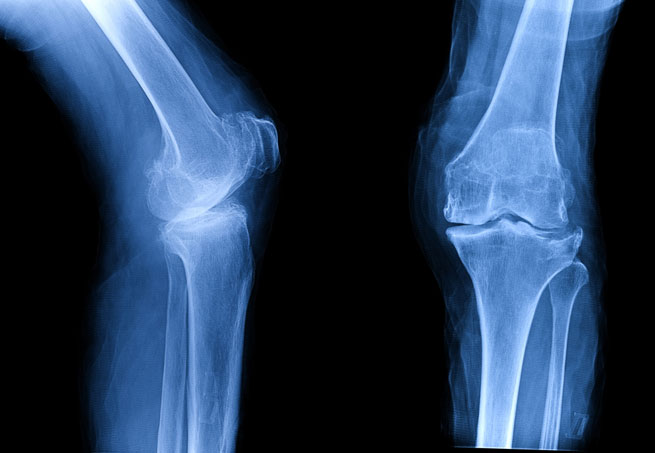
Osteoarthritis (OA), sometimes referred to as “wear and tear” arthritis, results when cartilage that cushions the joint degenerates and deteriorates. This leads to joint inflammation, pain, stiffness, and range of motion limitations. At its end stage, after significant cartilage wear and tear, OA may end in bone-on-bone arthritis.
What causes knee arthritis?
Risk of painful knee arthritis increases with age, obesity, prior trauma/knee injury, prior knee surgery, and repetitive stress to the joint often due to occupational or sporting demands.
How is knee arthritis diagnosed?
Patients with knee arthritis typically present with knee pain that is worsened with standing, walking, or increased physical activity. Physical examination may demonstrate limited and painful knee range of motion, stiffness, tenderness, or swelling. X-ray, computed tomography (CT), or magnetic resonance imaging (MRI) may aid in confirmation of diagnosis.
How is knee arthritis treated?
Initial treatment options for management of knee arthritis may include medications and physical therapy. Physical therapy should primarily focus on hip, glute, quadriceps, and hamstring strengthening. If a patient is still experiencing significant pain despite the aforementioned treatment options, interventional options may include corticosteroid (cortisone), hyaluronic acid (gel), or platelet rich plasma (PRP) injections. Finally, referral to orthopedic surgeon skilled in knee arthroplasty may be considered for further evaluation and consideration of surgical intervention.
Corticosteroid Injection
Using ultrasound, a needle is carefully and precisely guided to the knee joint capsule. Once the knee joint has been accessed, a steroid solution is instilled through the needle and into the joint capsule to coat or bathe the joint with anti-inflammatory medication. This helps to decrease inflammation and, subsequently, decreases pain and improves function.
Hyaluronic Acid Injection
Using ultrasound or x-ray (fluoroscopy), a needle is carefully and precisely guided to the knee joint. Once the knee joint capsule has been accessed, hyaluronic acid is instilled through the needle and into the joint. Hyaluronic acid is a component of synovial (joint) fluid and provides viscosity and elasticity. It may also have anti-inflammatory properties. This allows for restoration of joint lubrication and shock absorbing capacity with subsequent reduction in pain and improved overall joint function.
Platelet Rich Plasma (PRP)
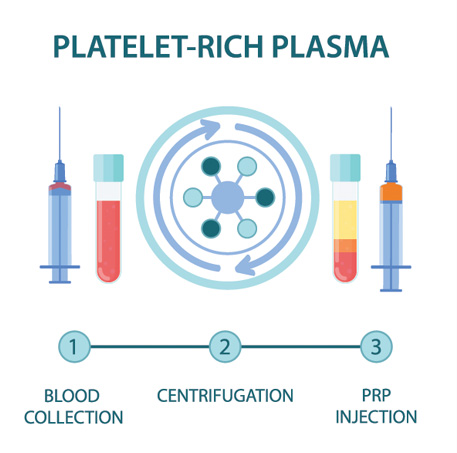
PRP is component of the patient’s own blood. It is rich in growth factors and other cells that signal an increased healing response to a damaged tissue. It is used to treat a variety of painful spine and musculoskeletal conditions.
Blood is drawn from a patient and then placed in a centrifuge for it to be “spun down.” This causes the different components of the blood to separate out in the vial. The PRP solution is then drawn up into a syringe and prepared to be injected at the site of the patient’s injury.
Discontinue use of all non-steroidal anti-inflammatory drugs (NSAIDs) at least 7 days prior to the procedure. These may include ibuprofen (Advil, Motrin), naproxen (Aleve), meloxicam (Mobic), diclofenac (Voltaren), indomethacin (Indocin), and celecoxib (Celebrex). If you are taking oral corticosteroids such as prednisone or a Medrol Dosepak, please discuss this with Dr. Best prior to your procedure. In some cases, Dr. Best may request that the corticosteroid medication be discontinued in preparation for the PRP injection. Do NOT stop aspirin unless specifically instructed by Dr. Best. Depending which body part is injected, you may need a driver to and from your procedure. If you have any questions or concerns about whether to continue or discontinue any of your medications leading up to your PRP injection, please discuss these issues with Dr. Best and his team.
Once the PRP solution is created, the patient is positioned for the procedure. The skin is thoroughly cleaned and the target for the injection obtained with ultrasound or fluoroscopy (x-ray). Then, a numbing solution is injected at the skin and subcutaneous tissues for increased procedural comfort. Finally, under ultrasound or fluoroscopic (x-ray) guidance, the needle is guided to the injury site and the PRP solution is deposited.
It is common to experience mild to moderate pain or discomfort during the initial 0-3 days after the PRP procedure. Post-procedure pain can be easily managed with acetaminophen (Tylenol) or other non-NSAID pain medication. Try to avoid applying ice or heat to the injection site.
During the 3–14-day period after the PRP injection, you may gradually increase physical activity. Please continue to avoid use of NSAIDs; however, ice may be applied for short periods of time throughout the day to aid in management of post-procedure soreness/discomfort if present.
During the 2–4-week period after the PRP, Dr. Best may recommend initiation of a course of physical therapy to aid in recovery and optimization of healing. The patient may begin to note improvement in pain during this time period, though it often takes 1 month or more for the benefits of PRP to take hold.
At this time, PRP injections are not typically covered by any insurance companies. Pricing and payment options can be discussed with Dr. Best and his team prior to your procedure.
As an alternative to PRP injections, intra-articular knee joint injections with corticosteroid or hyaluronic acid (gel) can be performed to help alleviate knee region pain. Using ultrasound, a needle is carefully and precisely guided to the knee joint capsule. Once the knee joint has been accessed, a steroid solution or hyaluronic acid (gel) is instilled through the needle and into the joint capsule.
Genicular Nerve Blocks and Radiofrequency Ablation
When a person’s knee joint is emanating pain, the genicular nerves will sense this pain signal and transmit it along a pathway to the spinal cord and up to the brain where we interpret and “feel” that painful sensation. As such, genicular nerve blocks can be used as a diagnostic/prognostic injection to help determine whether or not a patient may be a candidate for treatment with radiofrequency ablation (RFA). Using x-ray (fluoroscopy), needles are safely guided to and placed near the genicular nerves which are then anesthetized, thus temporarily blocking the pain coming from the knee joint. Patients are then asked to monitor their pain during the time period that the local anesthetic (numbing medication) is blocking the knee joint pain. In patients who experience a significant improvement in their pain, RFA of the genicular nerves can then be performed as a treatment to provide long lasting improvement in the pain. In patients who do not experience much improvement in their pain during the anesthetic phase, it can be determined with much more certainty that they would be unlikely to benefit from the RFA procedure and other treatments options would then be considered.
In patients who experience significant improvement in knee pain with genicular nerve blocks, they may then be considered for RFA of genicular nerves. Using x-ray (fluoroscopy), RFA needles are safely guided to and placed near the genicular nerves. The nerves are then anesthetized for improved procedural comfort. From there, the temperature of the needle tips is increased to perform the ablation of the genicular nerves during which they are essentially “cauterized.” This disrupts the pathway for the pain signal to travel from the knee to the brain, thus providing significant improvement in a patient’s knee pain.
At a Glance
Dr. Craig Best
- Harvard Fellowship-Trained Interventional Spine & Sports Medicine Specialist
- Double Board-Certified in Physical Medicine & Rehabilitation and Pain Medicine
- Assistant Professor of Physical Medicine & Rehabilitation and Orthopedic Surgery
- Learn more

